
The acromioclavicular joint or AC joint is located at the top of your shoulder and is where your shoulder blade (scapula) meets the end of your collarbone (clavicle).
Arthritis occurs when the smooth glistening cartilage that lines the joint wears away.
AC Joint arthritis is not the same as shoulder arthritis. Doctors usually refer to glenohumeral joint arthritis as ‘shoulder arthritis’.
Your glenohumeral joint is actually your shoulder joint. Your shoulder is where the end of your humerus (upper arm bone) called your humeral head meets the part of your shoulder blade (scapula) called your glenoid.
Symptoms of AC joint Arthritis
If you have AC Joint arthritis, then you will have pain located on the top of your shoulder. The pain is usually a dull ache, but can be occasionaly sharp or burning.
The pain can be at rest, at night and during certain movements or activities. You may have pain especially sleeping on the painful shoulder.
Certain movements can be particularly painful:
- reaching across to touch the other shoulder
- raising your arm towards your head until your arm touches your head
What causes AC Joint Arthritis?
AC arthritis is usually the result of repeated movements that wear away the cartilage surface found at the acromioclavicular joint. Because the shoulder is used so often, it is not surprising that after years of use the joint surface may wear thin.
Degeneration and arthritis of the AC Joint is often seen as part of the normal aging process. Occasionally, it becomes painful, but not always.
Certain injuries, such as AC joint dislocation or fracture-dislocation, can contribute to the development of AC arthritis.
Although AC joint pain commonly occur in together with other shoulder problems, such as shoulder impingement, bursitis and rotator cuff tears, they may occur in isolation.
Risk factors for developing AC joint Arthritis
The risk factors for developing arthritis of your AC joint include:
- Injury. If your have previous injured your AC joint by dislocation or fracture, then you are at higher risk.
- Age. AC joint arthritis is more common the older you get.
- Certain jobs. Jobs which involve repetitive activties with your arm above your shoulder height can predispose to AC joint arthritis.
Investigations
MRI
An MRI is also a very useful investigation, as it identifies other problems such as rotator cuff tears and bursitis, which are common with AC joint arthritis.
Xray
AC joint arthritis can easily be diagnosed by a simple Xray.
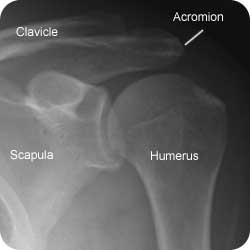
A Xray of the Left Shoulder showing normal anatomy
How is AC arthritis usually treated?
How is AC arthritis usually treated?
Treatment of AC arthritis depends on how severe your pain is.
Mild to Moderate Pain
Pain that is mild can be treated with anti-inflammatory medications and physiotherapy. Surgery is not needed if your pain is only mild.
Avoiding movements that hurt you is particularly important.
Physiotherapy can also be very useful.
Severe Pain
If your pain does not improve despite changing your activities and movement, tkaing anti-inflammatories and physiotherapy, then surgery may be necessary.
The surgical procedure involves removing the end of the clavicle (collar bone), and allowing the AC joint to fill with scar tissue. This allows for normal movement of the AC joint (which is minimal even in normal shoulders), and removes the rubbing together of the arthritic bone ends.
The surgery may be performed through a small incision directly over the joint or by key hole shoulder arthroscopy
Arthroscopic Excision of the AC Joint
Two small 1 cm incisions are made in the front and back of your shoulder. The camera (arthroscope) and small instruments are passed into your shoulder to remove the end of the bones.
Usually less than one centimeter of bone is removed to alleviate the pain of the AC arthritis.
For an isolated AC joint resection, treatment usually lasts about 8 weeks and often involves working with a physiotherapist. You are usually in a sling for 2 weeks to allow your wounds to heal properly and to allow your shoulder swelling to decrease.
If other procedures are performed at the same time, then your recovery may be longer.
-
FAQ’s
How long will I be off work?
That depends on your type of work and what modified activities are available at your workplace.
If you operation is only for your AC joint arthritis (as opposed to combined with other procedures such as repair of your rotator cuff), then you will be in a sling for 2 weeks.
Often, you can return to work after a few days, when your pain has settled.
If your work involved manual labour or overhead activities, you may need 6 weeks or more off work.
Further Reading and References
- Direct arthroscopic distal clavicle resection: a technical review. Iowa Orthop J. 2005;25:149-56.
-
Chronic shoulder pain: part I. Evaluation and diagnosis. Am Fam Physician. 2008 Feb 15;77(4):453-60.
