Knee Arthroscopy (Keyhole Surgery)
Knee arthroscopy is a minimally invasive procedure that allows us to diagnose and treat problems inside the knee through two very small incisions. A high-definition camera (arthroscope) is inserted through one incision while precision instruments are inserted through the other.
It’s one of the most common knee procedures and can address selected meniscal, cartilage, and ligament problems.

What conditions can be treated with knee arthroscopy?
Knee arthroscopy can be effective for selected problems, including:
- Torn meniscus: the meniscus is a C-shaped shock absorber. Tears (often sport-related) can cause catching, clicking or locking. Depending on tear type and vascularity, the meniscus may be repaired or selectively trimmed (meniscectomy) during arthroscopy.
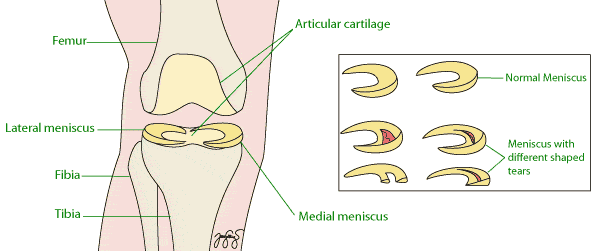
- Loose bodies: fragments of cartilage/bone that float within the joint causing pain, clicking or locking — removable arthroscopically.
- Chondroplasty (cartilage smoothing): trimming frayed articular cartilage to reduce mechanical irritation (does not regrow cartilage).
- ACL reconstruction: the ACL can be reconstructed using arthroscopic techniques.
Does knee arthroscopy help osteoarthritis?
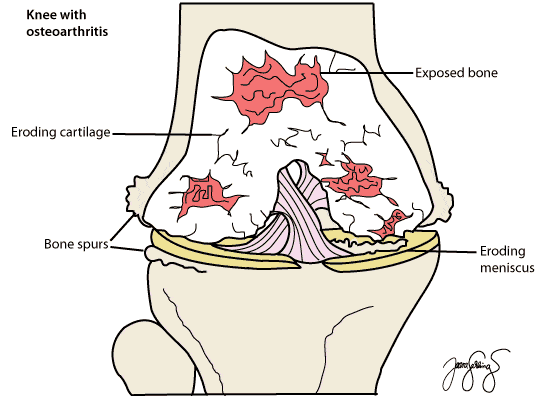
For advanced osteoarthritis, arthroscopy has limited benefit. If your knee is primarily “worn out”, the operation most likely to help is a total knee replacement. However, if you also have a treatable meniscal tear or loose body, arthroscopy may be considered for symptom relief.
Arthroscopy vs Knee Replacement for Osteoarthritis
| Aspect | Knee Arthroscopy | Total Knee Replacement (TKR) |
|---|---|---|
| Primary goal | Address mechanical issues (meniscal tear, loose body, focal chondral flap). | Replace worn joint surfaces to relieve arthritis pain and stiffness. |
| Best suited for | OA with clear mechanical symptoms and a treatable lesion. | Moderate–severe OA with global pain, stiffness, functional limitation. |
| Pain relief | Variable; good if symptoms due to treatable lesion. Limited for diffuse OA pain. | High likelihood of substantial relief for arthritis-related pain. |
| Recovery time | Days–weeks for most activities. | Weeks–months; structured rehab required. |
| Durability | No change to overall OA progression. | Prosthesis longevity commonly 15–20+ years (patient- and implant-dependent). |
| Risks | Low overall; bleeding into joint, stiffness, CRPS (rare). | Higher surgical magnitude; infection, clots, stiffness, implant risks (rare). |
| Typical next steps | If OA progresses or pain persists → consider definitive OA management. | Long-term follow-up; activity modification and strengthening. |
Key take-home: When osteoarthritis is the main problem, TKR is the procedure that consistently relieves pain and restores function. Arthroscopy is only considered if there is a specific mechanical lesion (e.g., displaced meniscal tear or loose body) driving symptoms.
What happens during a knee arthroscopy?
Admission
Most patients are admitted on the day of surgery and go home the same day.
Anaesthesia
You’ll meet the anaesthetist to choose the most appropriate option:
- General anaesthetic: asleep throughout (most common).
- Spinal anaesthetic: numbs the legs; a light sedative can help you doze.
If you have questions about anaesthesia, please contact your anaesthetist using the details provided.
The Operation
Two ~1 cm incisions are made at the front of the knee: one for the camera and one for instruments. The joint is examined and any treatable problems (e.g., trimming/repairing meniscus, removing loose bodies, smoothing frayed cartilage) are addressed. Sterile fluid flows through the joint for clarity.
Skin is closed with Steri-Strips or a few sutures if swelling is significant. The procedure usually takes 20–40 minutes.
Recovery Room
After surgery you’ll be monitored in recovery until awake and comfortable, then discharged with clear instructions.
How to prepare for a knee arthroscopy
Preparing your skin
Please let us know if you have any skin infection, rash or irritation near the knee prior to surgery.
Home support
You’ll be able to walk soon after surgery, but arrange help for the first few days with shopping, cooking, and laundry. If you live alone, we can discuss a short inpatient stay (subject to availability).

Recovery after a knee arthroscopy
You’ll go home with pain relief for the first few days. Keep the leg elevated initially to limit swelling and ice regularly during week one.
Begin gentle range-of-motion and quadriceps activation in the first two weeks to avoid stiffness. **Light cycling** is often helpful for swelling and mobility.
Wound care
Keep dressings intact for 7 days unless otherwise directed.
Rehabilitation
Your physiotherapist will provide exercises to restore flexibility, strength, and balance. Adherence to the program is key to the best outcome.
Back to work & sport
- Desk work: often within 3–7 days (if pain controlled).
- Manual duties/high-impact sport: usually 4–6 weeks, depending on findings and tasks.
- ACL reconstruction: has a longer, structured recovery timeline — see our ACL protocol.
Driving
Many people drive after a few days, depending on which leg was operated on, procedure type and pain control. You must be able to perform an emergency stop safely.
What are the possible risks and complications of knee arthroscopy?
The overall complication rate following knee arthroscopy is low. Potential risks include:
| Category | Examples | Comments |
|---|---|---|
| Expected effects | Soreness, temporary swelling | Common for days–weeks; improves with rest, ice, elevation. |
| General surgical | Anaesthetic reaction, infection, bleeding/haematoma, DVT | We use sterile technique, antibiotics when indicated, early mobilisation and DVT prevention strategies. |
| Arthroscopy-specific | Haemarthrosis, postoperative stiffness, CRPS, very rare iatrogenic cartilage/ligament injury | Early guided rehab helps minimise stiffness; persistent concerns are reviewed promptly. |
When to seek urgent help
- Fever > 38 °C, spreading redness or warmth around wounds
- Rapidly worsening pain/swelling, calf pain or new one-sided leg swelling
- Shortness of breath, chest pain, or coughing up blood
Further Reading and References
