Arthroscopy of the Knee, Hip & Shoulder
Minimally invasive “keyhole” surgery to diagnose and treat joint problems with
less soft-tissue trauma, clear visualisation, and faster rehabilitation.
What is Arthroscopy?
Arthroscopy is a minimally invasive technique that uses a high-definition camera and specialised instruments inserted through small incisions to diagnose and treat joint conditions. Compared with open surgery, arthroscopy can reduce soft-tissue disruption, allow precise treatment under direct vision, and support faster, safer rehabilitation.
Benefits of Arthroscopy
- Smaller incisions & soft-tissue preservation for less pain and swelling.
- High-fidelity diagnosis with direct visual assessment of cartilage, ligaments, and labrum.
- Day-case or short-stay pathways for many patients.
- Quicker return to function with structured rehabilitation.
- Lower infection risk compared with larger open exposures (when clinically appropriate).
Knee Arthroscopy
We perform knee arthroscopy to diagnose and treat intra-articular pathology such as meniscal tears, loose bodies, synovitis, chondral lesions and selected patellofemoral disorders. In appropriate cases, arthroscopy can alleviate mechanical symptoms (catching/locking) and reduce inflammation to help restore confident movement.
Common Indications
- Meniscal tears (traumatic or degenerative) requiring repair or partial meniscectomy.
- Chondral damage suitable for debridement, stabilisation, or biological adjuncts where appropriate.
- Anterior knee pain due to synovitis, plica or focal cartilage pathology.
- Loose bodies or osteochondral fragments causing locking or swelling.
Procedure Overview
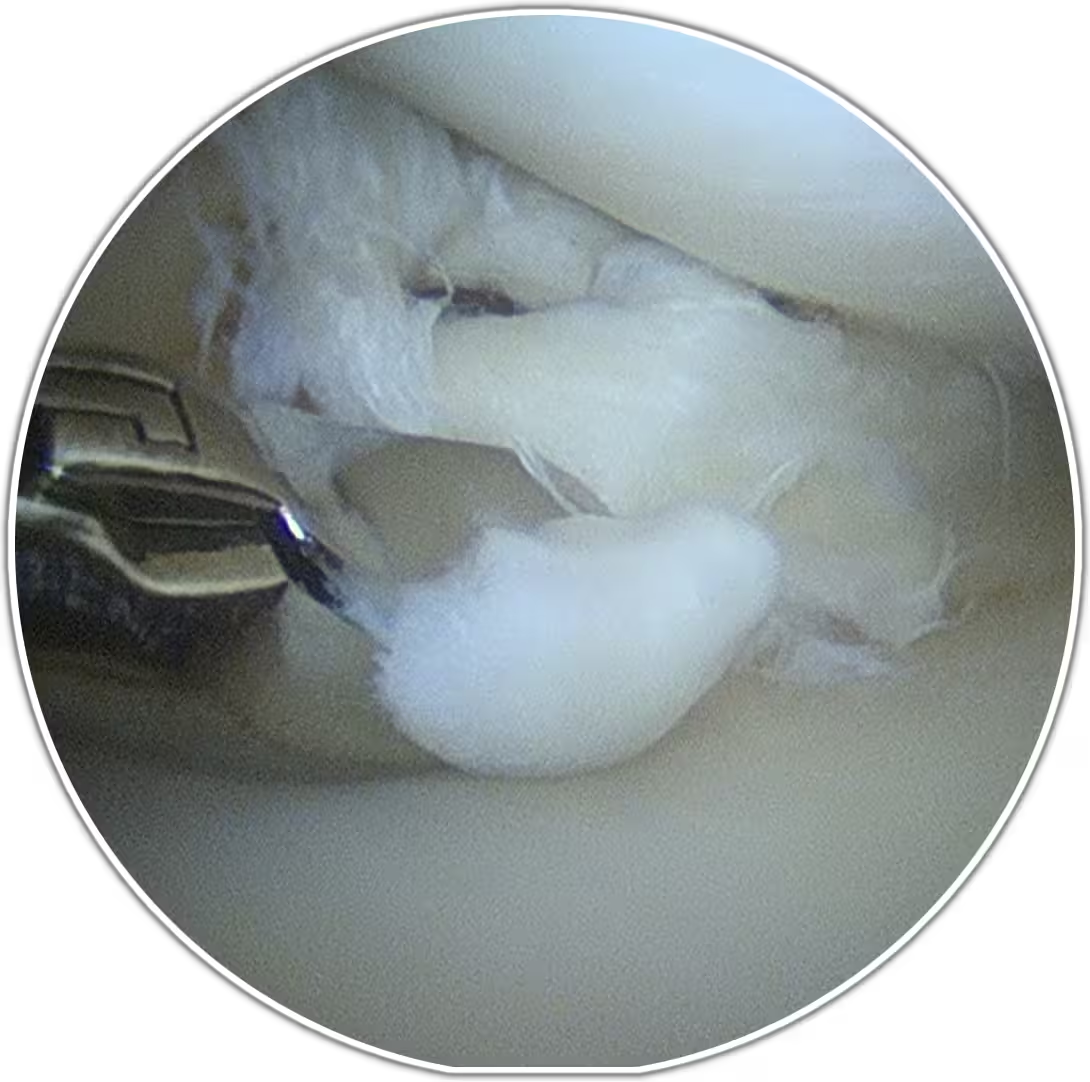
Through 2–3 small portals, the knee is inspected systematically. We treat meniscal pathology (repair when viable to preserve tissue) and address cartilage or synovial issues as indicated. Where possible, we prioritise tissue preservation to support long-term joint health.
Related internal links:
Knee Surgery Overview |
Knee Conditions |
Book a consultation
Hip Arthroscopy
Hip arthroscopy treats intra-articular pathology such as labral tears, femoroacetabular impingement (FAI), ligamentum teres lesions, and selected cartilage injuries. Our approach emphasises labral preservation/repair and impingement correction (cam and/or pincer) to restore the hip’s suction-seal and smooth range of motion.
Common Indications
- FAI (cam/pincer/mixed) with labral pathology affecting function.
- Isolated labral tears with mechanical pain; emphasis on repair over debridement when feasible.
- Ligamentum teres tears causing instability or persistent pain.
- Chondrolabral junction injuries suitable for stabilisation.
Procedure Overview
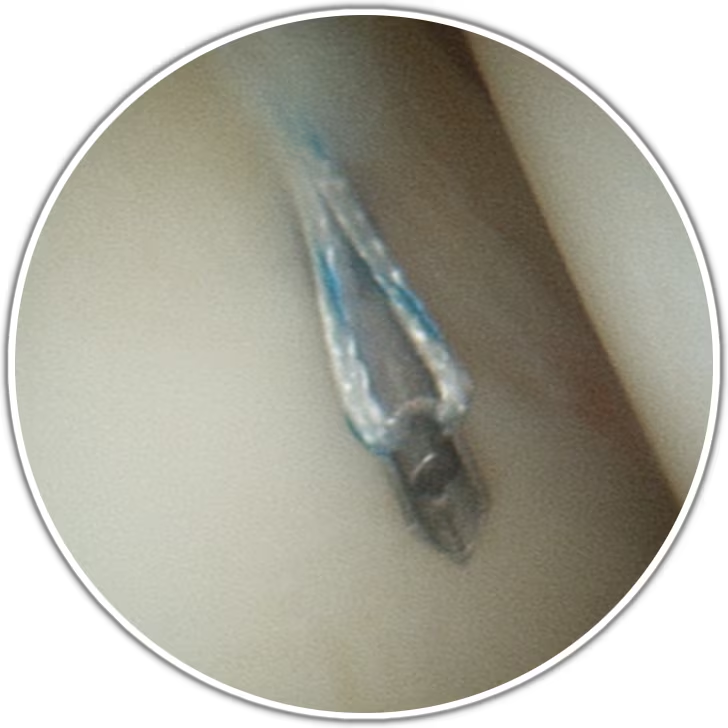
Through small portals, we visualise the acetabular rim, labrum, and femoral head-neck junction. When indicated, we perform labral repair and cam/pincer resection to relieve impingement and protect cartilage. Early, guided rehabilitation supports return to daily activities and sport.
Related internal links:
Hip Arthroscopy – Full Guide |
Hip Surgery Overview |
Hip Labral Tears
Shoulder Arthroscopy
Shoulder arthroscopy enables diagnosis and treatment of rotator cuff tears, subacromial impingement/bursitis, labral tears (e.g., Bankart/SLAP), and instability. We tailor care to your goals—pain relief, function, and return to work or sport—while protecting the deltoid and dynamic stabilisers.
Common Indications
- Rotator cuff tears requiring arthroscopic repair.
- Recurrent instability treated with labral repair and capsulolabral stabilisation.
- Subacromial pain from bursitis/impingement managed with bursectomy ± acromioplasty.
- AC joint or biceps pathology assessed and addressed as indicated.
Procedure Overview
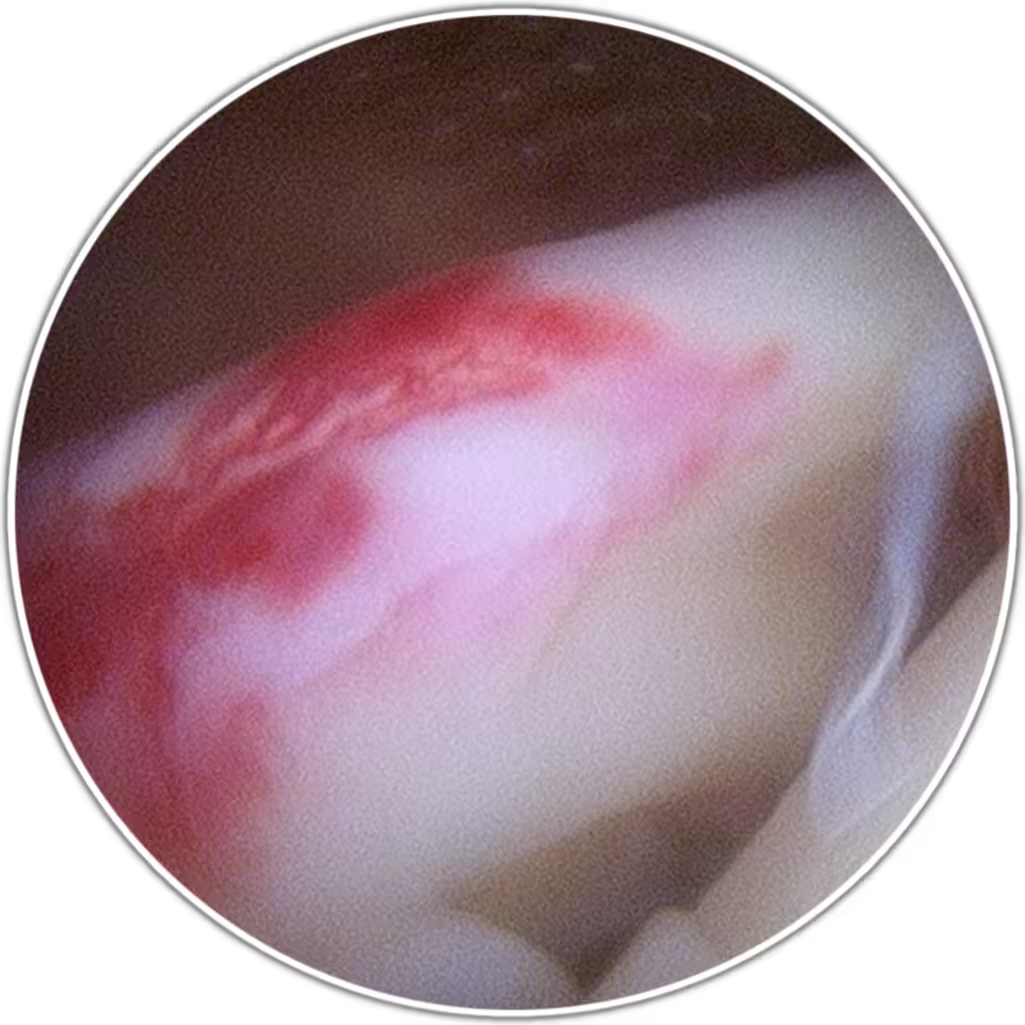
Using posterior and lateral portals, we assess the glenohumeral joint and subacromial space. Where suitable, arthroscopic repair of the rotator cuff and labral stabilisation are performed through small incisions, followed by structured rehabilitation.
Related internal links:
Shoulder Surgery Overview |
Rotator Cuff Tears |
Ask a question
Preparation, Anaesthesia & Enhanced Recovery (ERAS)
Outcomes improve when we combine patient education, prehabilitation, optimised anaesthesia/analgesia, and early mobilisation. Many arthroscopy patients are suitable for day surgery with rapid return to home supports.
- Prehab: targeted strength, mobility and swelling control strategies before surgery.
- Anaesthesia: general or regional anaesthesia plus multimodal analgesia; for shoulders, a regional block may improve comfort immediately post-op.
- Early rehab: joint-specific protocols guided by our physiotherapy network.
- Return to work & sport: staged progression aligned with tissue healing and objective milestones.
Related internal links:
Enhanced Recovery After Surgery (ERAS) |
Patient Information |
Day Surgery Pathway
Risks & Considerations
All procedures carry risks. We discuss your specific risk profile during consent, including measures to mitigate complications.
- Bleeding, infection, or thrombosis (DVT/PE risk tailored to patient factors).
- Nerve or vessel injury (rare) and portal-site issues.
- Stiffness, persistent pain, or progression of underlying degenerative disease.
- Re-tear or non-healing risk for tendon or labrum repairs depending on tissue quality and rehab compliance.
Recovery Timeline (Guide)
Knee Arthroscopy
- Days 1–7: swelling control, gentle range of motion, early weight bearing as advised.
- Weeks 2–4: progressive strengthening and gait normalisation.
- Weeks 4–8: return to low-impact cardio; sport-specific drills as tolerated.
Hip Arthroscopy
- Days 1–10: protected mobility, range work within comfort; avoid impingement positions initially.
- Weeks 2–6: structured strengthening, gait retraining, gradual activity expansion.
- Weeks 8–16: return to running/pivoting per milestones and strength symmetry.
Shoulder Arthroscopy
- Immediate: sling or immobiliser if a repair was performed; early hand/wrist/elbow motion.
- Weeks 2–6: guided passive/active-assisted shoulder range (protocol-dependent).
- Weeks 6–16+: progressive strengthening and functional return (work/sport staged).
Where We Operate & Access Options
We operate at leading Melbourne facilities with modern theatres and day-surgery capabilities. No-gap pathways may be available for eligible patients and procedures. Our team can help you confirm health fund eligibility and discuss short-stay/day-case plans where appropriate.
Related internal links:
Locations |
No Gap Orthopaedic Surgery |
Appointments
Ready to discuss arthroscopy?
Bring any previous scans and a list of your goals (work, sport, daily activities). We’ll tailor a plan around your priorities.
Arthroscopy FAQs
Is arthroscopy always the best option?
No. Some conditions are better managed with rehabilitation, injections, or open procedures. We recommend the safest, most effective option for your condition.
Will I need a brace or sling?
Knee patients rarely need a brace after simple procedures. Shoulder repairs often require a sling; hip procedures may need temporary movement restrictions. We provide a clear, written plan.
When can I drive and return to work?
Once you can safely control a vehicle and are off sedating medication—timeframes vary by procedure and limb. Desk duties may resume within days to weeks; manual work needs longer and staged clearance.
What about pain after surgery?
We use multimodal analgesia, icing, elevation and early physiotherapy to control pain and swelling. Discomfort typically improves over the first 1–2 weeks for knee and several weeks for hip/shoulder repairs.
External Links & References
- AAOS OrthoInfo — Arthroscopy Overview
- NICE Guidance (UK) — Musculoskeletal Procedures
- British Journal of Sports Medicine (BJSM) — Rehabilitation & return-to-sport frameworks.
- Arthroscopy: The Journal of Arthroscopic and Related Surgery
- PubMed — Peer-reviewed evidence on knee, hip and shoulder arthroscopy
Next Steps
Our East Melbourne team will help you decide if arthroscopy is the right choice and outline a pathway that fits your life and goals.
